STOMA CARE ADVICE
MOISTURE
You will breathe easier, cough out thinner mucus with less effort, and have a cleaner, healthier stoma if you will irrigate, use a humidifier, and keep your stoma covered to avoid losing moisture each time you exhale. If you are away from your humidifier, carry a small spray bottle with clean water and use it to spray your stoma and your stoma cover. Keeping this area moist is the secret to avoid any crusting (dried mucus in and around the stoma) and to keep any bits of dried mucus or blood from solidifying inside your trachea. If you are crusting or coughing up dried bits, add more moisture. Being well hydrated by drinking plenty of liquids is also a important in keeping the mucus softened.
Check our Stoma Dos and Don’ts for more hints on moisture or humidifying. You can also refer to the Stoma Care Equipment section for more information on Humidifiers.
USE A GOOD STOMA FILTER
It is a good idea to keep your stoma covered to help keep out dust, pollen and other contaminants. There are several options for covers including foam filters available from many vendors. You can use a stoma bib as described in the Stoma Covers section or an HME (Heat Moisture Exchange) filter discussed in the HME section.
1. For laryngectomy patients, like myself, living on the Gulf Coast, low relative humidity is seldom a problem unless you happen to share air-conditioned office space with numerous electronic office automation devices. Facility managers tend to crank down ambient moisture to insure long life and proper function for these non-human contributors. In this situation and lacking a functioning nose and sinus passages, you will have an annoying little problem that will not effect your co-workers. Not only is your body tricked into believing you are working in Death Valley, but the lower humidity contributes to additional airborne particulate material. “Paperless office” is still very much an oxymoron and there is plenty of paper dust to take flight in the artificially dry air. The result – A significant increase in mucus production while you are at work. Not something you really need while trying to blend in. How do you remedy this discomfort when environmental changes are clearly beyond your span of control? Simple – If you can’t change your environment, you change yourself. First, super-hydrate by drinking more water than a fish. Forget trying to count and comply with the dumb eight glasses-a-day rule, just drink water until your urine begins to clear. To avoid constantly beating feet to the water fountain, keep a water jug and stadium cup at your desk. After a while, all this additional water intake merely becomes part of your daily routine. You may wish to cut out or at least cut back on coffee consumption. The only way to defeat airborne crud is to have very, very good stoma filtration. There are a number of fine products on the market, but at this point, my personal favorite is the PROVOX Stoma filter. When I discard a filter cassette, you would not believe what that little devil has intercepted for me. In addition to keeping bad stuff out, good filtration also slows the escape of moisture from your respiratory system. Everyone is different, but this should reduce your mucus production to manageable levels while you are at work and allow you to return to your former level of productivity. Unless you are looking for a reason, a laryngectomy should not force you into retirement. (Marvin Whitley)
2. I had an experience with what we breathe in, while wearing a white crocheted stoma cover and working in the garage on planting some flowers in new pots. Put potting soil in them. Later when I went in the house, there was a perfect black circle on my white stoma cover where it had caught the dirt in the air I was breathing. So anything over the stoma helps to filter.
Also a friend told me before he went to mow the yard, he always wet his stoma cover down so it would catch the dust and pollen.
Pat Sanders
DAILY CARE
Daily care is needed to prevent infection and skin irritation, especially on a new stoma site.
Caution must be used to never use anything other than water based products in or around the stoma. Caution should also be used to prevent lint from tissues from entering the stoma or lungs. Saline solution can be used to help soften the mucus enabling it to be removed easier. You can make your own or use the pink saline bullets available. It is always better if you can cough out the mucus to clear your lungs however if this is not an option for you, you may have to use a suction machine.
(More detailed information can be found in Stoma Care – Dos and Don’ts.)
(Additional information on stoma care, humidifiers and suctioning can be found at: Equipment
CATCH THE SNEEZE
When you cough or sneeze and don’t get covered in time, the result can be embarrassing when projectile mucus flies from the stoma. Avoid this by using a stoma cover or at least something like a foam square. This will protect your clothing and keep foreign items, like a flying bug, from entering your stoma. In the unlikely event that this occurs, a little squirt of saline solution or plain water in the stoma will help to cough it out.
TEE SHIRTS
One of the most irritating, exasperating things about my stoma was when clothing like crew neck tee shirts blocked my stoma from time to time. V-neck tee shirts are a welcome relief and make it much easier to get to the stoma for cleaning.
TEMPORARY STOMA VENT
If you lose your stoma vent (tube) and don’t have a spare, it may take a few days to get a new one. If it is urgent that you wear one (as in stoma stenosis), use a baby bottle nipple, cut the narrow tip back to increase the inner diameter and it will make a temporary short tube. The flange end could be pierced on each side and you could use ribbon, string, or shoe laces to tie behind the neck and hold it in the stoma. You can even sterilize it before and after use. (Judy Greiwe)
OTHER PROBLEMS
Don’t be too quick to assume that you will not use a stoma vent that you have quit wearing or electrolarynx that you think you will not go back to. Keep a box of spare items as a “just in case” supply box.
READING REFERENCES
In March, 2005, we published, in Whispers on the Web, the first 10 of 100 hints, called Living the Lary Lifestyle. We continued for the next 9 months with 10 new tips every month including interesting comments by the author next to each hint. You will find green links to each of the newsletters of that group below. You will be amused, educated and delighted. If you have time and as long as you are there, you might take a look at other articles of significance to you.
Pat Sanders
Living the Lary Lifestyle – Joan G. Burnside, M.A.
INTRODUCTION
Welcome new Lary! These tips represent my learning process during the year following my laryngectomy with the help of the WebWhispers on-line support group and the Speech Pathology staff at MD Anderson Cancer Clinic and Hospital in Houston. I hope the tips will give other new Larys a jump-start on the road to a new life and remind experienced Larys of just how far they’ve come.
I am grateful to all the WebWhispers members for sparking many of these tips and for welcoming my contributions and questions on the web. I am indebted also, to the speech-language pathologists at MD Anderson because their admirable service inspired me to expand and update my speech-language pathology background.
These tips have been written from the viewpoint of a patient and are intended only as a supplement to the professional advice and treatment offered by physicians and speech-language pathologists who specialize in the treatment of laryngectomees.
Joan Burnside, MA
College Station, Texas
February 2005
Do’s and Don’ts
DO – ADD HUMIDITY
(For recommendations on Humidifiers, check Stoma Care – Equipment)
RULES CONCERNING HUMIDITY
Humidity is important to a laryngectomee but there limits to
maintain. The relative humidty should stay between 30-55% except when in
the shower. Remember that relative humidity is not the same as
humidity. Relative humidity refers to the amount of water that air can
hold at a certain temperature. Air temp at 75 degrees may have a cup of
water in the air at 100% RH while at 40 degrees it may hold only a 1/4
cup at 100% RH.
Rules concerning humidity are simple:
1. Get a gauge that tells you the relative humidity. They can be found
at Walmart, Amazon and many other places especially if they have garden
centers.
2. Keep the range between 30-55% relative humidity. Below 30% the air
becomes hard to breath and dry skin conditions, along with other
problems, form. 60% and above constantly maintains an environment
desired by mold.
3. If moisture forms on the inside windows you may have one or both
problems of needing new windows and/or the humidity level is to high.
4. If you still have breathing problems at 55% you need to talk to your doctor about breathing therapy.
5. If you have a central air heating and cooling system find a good
HVAC company to install a humidifier for you. If you don’t have one of
those systems, then carefully look into of the shelf tabletop/tvstand
units. Even with an central air system, monitor that areas that you
spend the most time in as the bedroom. You may need a small unit in that
area too.
Frank O, Croydon, Pa
PERCENTAGES
I live in Minnesota and have found anything over 30% humidity is
within my comfort zone. I only use a humidifier during the winter
months. I keep it in the 30 something % range on my homes main floor
which results in the 40 something % range on the second floor where my
bedroom is located. Theoretically my attic will be in the 50 something %
range as the moisture seems to rise. This should keep any mold from
forming in my attic as that is supposed to happen around 60 – 65%. I
have a humidifier in my office that I use during the day. I have several
gauges in my home so I can monitor the % and adjust as necessary.
Wild Bill, – MN
WAYS TO HUMIDIFY
In my one-bedroom apartment I have a
humidifier in the living room, another in my bedroom, I live right on
Lake Erie but the winters tend to be dry and cold, and believe me, these
help. Come summer, when the air conditioner is on, makes no sense for
any of that: The AC has a de-humidifier built in and, with the Lake
right outside, moisture a-plenty.
John S. – Ohio
WORKS WITH YOUR SHOWER
In the Cold weather, humidity control is important. I have used every kind of humidifier I could get my hands on. In my opinion, the Mr.Misty is the best. The principle of the units operation is the water pressure in your shower. You simply screw the shower head off and screw Mr.Misty on in it’s place. You then screw the shower head on the Mr.Misty unit. When you turn your shower on, there is a very fine mist that comes out of the unit. When you are ready to shower all you have to do is push one button on the Unit and you have a regular shower. This unit puts more than enough moisture into the air with no filters or messy units to clean or replace. It is not automatic and you will need a meter to watch the humidity level. The moisture will naturally spread to every room. I purchased mine in my local drugstore and it works so simple and good I am amazed any time I turn it on. I am just over my first year and believe my life get easier and better every day that the good Lord gives me. If you have any questions you can reach me by e-mail in sunny but cold Florida.
Ron Momeyer (Note from Editor. I was not able to find these online)
HUMIDITY – INTERNAL & EXTERNAL
I would hate have beat the big “C”, for as long as I have, then die from coughing. The ideal objective for lary mucus is to have a continuous flow of watery, almost clear mucus. Like mucus elsewhere in your body, that which is produced in the respiratory system protects the tissues of the trachea (stoma hole and tube down to the lungs) and lungs which are exposed to the dirtier, colder, and drier air (since the upper part of our respiratory system became bypassed by the laryngectomy surgery.) In addition to providing a protection of the tissues to prevent drying and the invasion of bacteria and viruses, the upward mobility of the mucus carries any impurities which are breathed in up so we can cough them out. Managing the amount of mucus used to be an automatic process before we became larys, but now we must play a more active part. Things we have to actively do to get and maintain a good consistency and flow of mucus (basic):
1. Hydrate yourself. Do not just drink water when you are thirsty, but drink enough water and other liquids during the day because water from your body is the building material for the formation of protective mucus.
2. Keep the humidity in the spaces you control at about 50% relative humidity (certainly no higher than 55%). If you have an automatic whole house humidifier, your job is easy. You just set the humidity level like you set the temperature with your thermostat. The rest of us have portable humidifiers and humidity gauges to check it. You can buy portable humidifiers which have an automatic on and off function when they reach the set humidity, but they are not inexpensive.
3. Wearing an HME (Heat/Moisture Exchange) filter raises the humidity and heat of the air you breathe by temporarily storing both in the filter when you exhale, and returning it to the lungs when you inhale again. The filters are also excellent at filtering out the impurities found in the air around us we breathe.
4. While we disagree about whether it should be a daily ritual or only used occasionally or as used, squirting some sterile saline into your stomas can help loosen by thick mucus and help you cough it up. A product like the pink saline bullets serve this purpose.
5.The saline bullets are the safest way to go But, if you’re going to buy over the counter saline, check the ingredients! The only ingredients should be sterile water and salt.
6. You can also add additional humidity at the stoma level by dampening a cloth (the double lined ones like the Gennel are particularly good) or foam stoma patch. When you travel in your car, or otherwise, you can carry a small spray bottle containing water to redampen your stoma cover. Whenever I fly, I bring or ask for a bottle of water and use that to keep the stoma cover wet. Doing so also improves the covers ability to filter impurities from the air.
7. You can also get some temporary relief from dryness when you take a steamy shower, breathe in the steam from a boiling teapot (don’t get close enough to get burned), or use a nebulizer.
David B. – VA
MOTHER NATURE USUALLY GETS THINGS RIGHT
Prior to the laryngectomy surgery the air which reached our lungs was almost always filtered completely clean, was 98.6 degrees Fahrenheit, and 100% relative humidity (think fog). The laryngectomy surgery bypassed the upper part of the airway which accomplished this conditioning of our incoming air and what we began to breath was dirtier, cooler, and drier. Too little humidity is unhealthy, as is too much. At either extreme the environment is ideal for the growth of respiratory infections, bacteria, dust mites, fungi, viruses and the like. Go to Possible Problems Section for more information on humidity. We can adjust to dirtier, cooler and drier air, but if you believe that Mother Nature tends to get things right, doing what we can to approximate our respiratory environment prior to becoming larys seems like the better idea.
David B. – VA
TOO MUCH OF A GOOD THING
Too much of a good thing? 50% relative humidity is about the maximum before the disadvantages overwhelm the advantages of additional humidity. There is an article, “Ideal Humidity Level,” with a chart which shows why too dry air or too wet is not healthy in this issue of the WW monthly publication: http://www.webwhispers.org/news/dec2000.htm As you mentioned, an excellent investment is a digital battery powered humidity gauge (hygrometer) (great holiday gift for a lary!) available from Wal-Mart, Amazon and many other locations.. However, during the winter months I find that I still must add more humidity at the stoma level by dampening my stoma cover with water or I will still dry out. It is less of a problem in the summer months.
David B. – VA
BUY SALINE SOLUTION
1. You can purchase sterile saline at your local pharmacy in large bottles to fill your own bottles or sprays. You can find it in small nasal spray bottles or in the contact lens care section of the store. Several manufacturers sell saline in a can for misting and you can purchase saline bullets. All of these things contain the same product. Amazon and pharmacies have an amazing selection including the pick bullets,
2. Sea water is 3.5% salt (I looked this up). Normal saline is .91%. When you swim in the ocean, yes, you’ll get the salt residue on your skin as you dry but the inside of your body is normally a bit salty–more like normal saline. When you shed tears, they are salty. If you need to flush out your eyes for any reason, plain water will sting. If you use normal saline, this will not sting (at least not as much). In the hospital, when they give IV’s, it is
usually normal saline that they give you to be close to the saltiness of your blood. Saline is also used to flush wounds but wound flushes have added ingredients.
Vicky M. WI
3. Saline Solution is used for eye wash, nasal irrigation, and stoma irrigation. Look under Google for Saline Solution, Find in Med supply places or our own vendors. Check your drug store and Walmart or Amazon. Read the labels closely and compare. Same or similar product, can differ on the ingredients.
4. I use bullets and always carry at least one saline 5 ml capsule in my pocket. When I start repeated coughing, I squirt 1/2 or all of it into my stoma. This seems to replenish the moisture in my lungs and the coughing stops. I keep these capsules in my jacket pockets, car glove compartments, my desk drawers at work and always one in my shirt pocket so they are always handy when I need them. I also start and end my days with 1/2 a capsule. I use 1/2 the capsule in the morning and the other 1/2 at night. These can be purchased without a prescription now due to some change in a Federal law. Walmart, Amazon and Target all carry them in the pharmacy. The container is also recyclable.
William C. – MN
5. Caution: There can be a lot things in common tap water that you do not want in your lungs or stoma. Boiling tap water might kill the bacteria but it does not remove the chemicals and particulates in the water. If you use water in any way in your stoma, use distilled saline water to make sure there are no additional things in the water. Read the label very carefully on any saline products. If in doubt discuss it with your doctor. Water can grow bacteria very quickly so discard what is unused. Better to be safe than sorry.
Ron M. – WA
AWAY FROM HOME
IN THE HOSPITAL
In the orders your doctor gives the hospital should include that your chart says “laryngectomee. Total neck breather. If oxygen required, apply to neck only”. If you use a TEP a note should also be attached to not remove it. The doctor’s orders should also inform the respiratory service at the hospital that you will require humidified air supplied continually with a trach mask which fits loosely around your neck. Suction should also be hooked up and ready for you to use or the hospital staff should it be needed. A sign close to your bed repeating the “laryngectomee. Total neck breather, etc.” would also be a good idea. And your chart should also read that you may not be able to speak. A placement close to the nurse’s station is an especially good idea for larys. If the hospital has a way to remotely monitor your oxygen saturation level at any time you are sedated that is still another layer of protection since this would indicate if your stoma had become plugged with mucus.
David B. – VA
IN THE CAR
In most cars you may change the ventilation system from “fresh air intake” to “recirculation of the air.” If you use the recirculation system, the humidity will increase immediately. If the windows mist up, the humidity will be near 100%, and it’s time for getting fresh air intake again. May be you find the right balance just with a small opening of one window? Not a good idea to bring a humidifier into a car!
Lorents G. – Norway
For more information on Car Safety, check the Safety Section.
IN AN RV
We travel and live in our RV for about 4 months each winter. RV’s traditionally use a propane furnace system for warmth and very frequently use a “cube” electric heater to supplement the RV furnace. Both of these heating devices take moisture from the air to well below an acceptable level of moisture. Last year we were introduced to a new space heater called the EdenPure. We were told it would not remove moisture from the air and would provide much more warmth than other heaters used to supplement the furnace. It is economical as well, using about half the electric of other supplemental heating devices.
This is our second winter using the EdenPure and I can tell you it does not remove moisture from the environment. In fact we are having to air out, even in this cold spell just to get dryer air in the RV. Cooking and showering produces more moisture than we need. We use it at home as well to heat our sun room, especially in the evenings after the sun has set.
I do not sell the product nor have any financial connections to the company.
Max
DON’T – USE OINTMENTS
QUESTION: Dr.. Peters, there was a big discussion recently in our WebWhispers online group about using ointments inside or around the stoma. What do you recommend in the use of antibiotic or antibacterial ointments
ANSWER: That’s a very interesting question. I think that if the stoma has “matured” or completely healed that nothing is needed. If a raw area develops from say using your speech prosthesis then a short course of an antibacterial is indicated until the area heals. I would not recommend a routine daily use of such products when nothing is wrong with the stoma.
I can think of three reasons that routine use should be discouraged. The first thing that comes to mind is that most antibiotic ointments have a petrolatum (ie petroleum) base. If a big “glop” of that stuff gets aspirated and finds its way into the lungs then a lung abscess could result.
The second has to do with the fact that the main function of having petrolatum in a medicine is that it makes a seal on the surface. That is why we use it on a fresh wound cause it seals the bad guys out. The other thing it does though is to seal moisture and any surface bacteria IN as well. This will create a situation that is chronically “wet” and actually damage normal skin.
The last thing has to do with resistant bacteria. When bacteria are chronically exposed to an antibiotic they mutate in such a fashion that they become immune or resistant to that drug. That is why antibiotics should always be used sparingly and only when truly indicated. The classic example of this is the horrible practice of prescribing antibiotics to treat a cold which is generally caused by a virus.
So, when you have to use an antibacterial medication to treat an area of irritation around your stoma, use it sparingly and use a water soluble CREAM that won’t risk damaging the lungs.
Glenn E. Peters, M.D.
What is in Ponaris? AmericanRx.com describes it as follows:
MANUFACTURER: BIOFILM
INDICATIONS: Ponaris Nasal Emollient for relief of nasal
congestion due to colds, nasal irritations, Atrophic Rhinitis (dry
inflamed nasal passages), nasal mucosal encrustations, and allergy
manifestations (Rose and Hay Fever). Ponaris is a compound of carefully
selected mucosal lubricating and moisturizing botanical oils specially
treated through the exclusive J-R Iodization process since 1931.
Exclusive Prescribed Therapy for: Colds (Sinusitis), Rhinitis (Acute,
Chronic, Allergic), Post Nasal Drip, Epistaxis (Bloody Nose) = due to
irritation of dried mucous membranes, Rebound sinus reaction from drugs
and smog.
INGREDIENTS: Oil of pine, Eucalyptus, Peppermint,
Cajeput, and cottonseed as specially prepared iodized organic oils.
Total iodine 0.5% to 0.7%. Assimilable hence non-lipoid potential.
Packing on sterile gauze.
DIRECTIONS: Instill half-dropperfuls in each nostril (fill to line on dropper) as needed, or as directed by a physician.
One ongoing concern for us all is the use of products designed and safety tested for one purpose being used by larys for another. Since we larys are so few in number it should not come as much of a surprise that there would not be many products specifically designed with us in mind or even safety-tested for our use. Many products which have been designed for use by non-larys to use by, for example, squirting into their noses, could be very unsafe to squirt into a stoma. The reason is our changed anatomies. For example, for a non-lary squirting a cold remedy product in their noses any excess is likely to end up in their stomachs and broken down by stomach acids and any waste products flushed out by the body’s incredible waste disposal system. The lungs, on the other hand, have very limited ways to get rid of contaminants, and squirting the products into the stoma could be a health hazard.
One way the lungs get rid of contaminants is to cough things out. But we know that larys often must take some conscious steps to keep their respiratory systems functioning well with an adequate amount and flow of mucus moving upwards.
One troubling fact is that the respiratory cilia (microscopic hairs which line the trachea and bronchi) which carry mucus and whatever contaminants are suspended in it upwards and out stop functioning when the relative humidity level in the respiratory system drops to 30%. And indoor humidity can drop this low, particularly during the winter. The mucus becomes too thick to be moved at all by the cilia. So contaminants suspended in the mucus remain in the respiratory system too long, and some of these contaminants and immobile mucus are associated with several diseases including emphysema and worse.
Many of us (certainly including me) abused our lungs for decades by smoking and breathing in lots of other garbage. As a consequence, I am pretty leery of introducing anything into my lungs via the stoma other than water vapor from my humidifier and dampened stoma covers.
David Blevins, Va
Equipment
YOU NEED TO SEE WHAT YOU ARE DOING
3X MAGNIFYING
A wall mirror over a sink with a flashlight just doesn’t work. One of the most essential things to have is a lighted 3X magnifying mirror. This is necessary to do a thorough cleaning job of the stoma and prosthesis.
A WELL LIT MIRROR
Since all of us with stomas spend considerable time caring for and
cleaning them, a well-lit magnifying mirror makes a difference. A makeup
mirror with lights on the sides helps. So will a small lamp that aims a
spot of bright light. Look in the catalogs with laryngectomee supplies.
LIGHTING
Lighted mirrors are available or you can use a small hand held flashlight. Hand held flashlights allow greater control of the light so you get the light directed into the deeper area of the stoma. LED light works well because they produce a bright light and little battery power.
Lamp and Mirror
Tom Warborg made this lamp for his wife Carol, for her stoma care.



The lamp is from Seattle Lighting, it is called LED’s by Zeppelin, Product No 422465, and costs about $55.
The mirror is Coghlan’s Featherweight from REI, costs $3.25.
The rubber washer and spacer are from the local hardware store. Cheap.
The beauty of the thing is it gives a very bright light, which can be shined right at the stoma, while the mirror above reflects the illuminated stoma, not the viewer, and mostly the hands and instruments are not in the way. Better than anything we have tried.
Tom Warborg
Note: these lamps are no longer available but I have one and it the best thing I have every used. You may be able to find a similar lamp to make your own.
Ron Mattoon Seattle 2010
Posted 10/ 2019
STOMA CARE – PERSONAL EQUIPMENT
A GOOD PAIR OF TWEEZERS
Following a laryngectomy, you will quickly pick up another little task to add to your morning routine of whisker removal, hair brushing, and dental hygiene. Yes – You’ll also have to remove that pesky, overnight, accumulation of mucus from the margin of your stoma and/or from your prosthesis. Get a good pair of tweezers. Instead of the drugstore, you need to check out the hardware store. There you’ll find a pair cross-bent electronic tweezers. They were intended as soldering aids, but you would think they were designed with us in mind. These are hefty, stainless steel guys over six inches long with straight and bent blades (I prefer the 45° angle), but the really neat thing is that they operate on negative pressure. In other words, you open them and when you release, they clamp down. This will allow you to concentrate all your effort in that gentle, strategic pulling necessary to effectively remove any hardened mucus. They will last you forever and the cost is a very nominal $2-$5.00. (Marvin Whitley)

MY CHOICE OF TWEEZERS
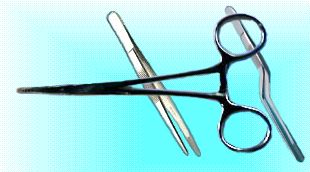
A good pair of tweezers is an essential tool for a lary. While I have a pair of the ones with the angled tips which I like, my favorite is the medical “hemostat” (or clamp). They look similar to a pair of scissors, but the ends are blunt and pinch together. They can also lock closed in a powerful grip via an overlapping set of metal teeth adjacent to where your thumb and forefinger go. You can order this from several laryngectomee suppliers, or can often find them in hobby, military surplus, or medical supply stores.
SUPPLIES KIT TO CARRY WITH YOU
1. I use a small camera case to hold a supplies kit. I use one that is zippered and fits into my pants pocket or jacket when I am going out of the house. I carry my spare HME filters, EL batteries, tweezers, HME base plate adhesive, etc. It is all in a small maintenance kit, along with a small package of paper tissues, has everything I need during my day.
2. Another option is using a glasses case. It can not only hold your reading glasses, but can hold a TEP brush, tweezers, and a small light. I use one that is a pen that has the light built into the end of it.
Ron Mattoon Seattle 2010
posted 8/2018
STOMA CARE – APPLIANCE OR MEDICAL EQUIPMENT
HYGROMETER
1. I had my surgery in February and was told to keep humidity high in the house. I was running 3 portable humidifiers, 24-7. The windows were soaked and the paint peeling off the walls under the windows. Result, I just spent a fortune to have damage repaired and the house painted. This year, I bought a small unit to measure humidity for $6 and keeping humidity to 50%. Seems to be working. I live in cold Canada, where it’s about 5 Fahrenheit this morning.
Joe S. – Ontario
2. A hygrometer will keep track of the humidity. You should try to maintain it in the 40% to 50% range, although a little less may not be a problem IF it doesn’t cause excess mucus and coughing. I have a Vicks that cost about $35 or $40 and, on low, I can hardly hear it with it placed within six feet of me.
Dave R. – FL 0807
OXYGEN NEEDED?
If you are having breathing problems, you might look at different types of breathing help. There are many companies that supply oxygen concentrators and equipment. This site will help you understand what equipment is available.:
https://www.rotech.com/respiratory-services/home-oxygen-therapy
Rotech’s education section will help answer other questions.
https://www.rotech.com/resources/patients/education
It explains how weather, humidity, barometric pressure, temperature and elevation affect your breathing.
We have a section under Possible Problems, Being on Oxygen with some items of interest.
Consult your doctor to see if oxygen is needed.
HUMIDIFIERS – EXPLANATION
There are basically two types of humidifiers that we use as laryngectomy patients. Of course, cleanliness is always a concern on both types of humidifiers to eliminate the growth of mold and bacteria.
1. The household appliance type is used to increases humidity (moisture) in a single room or in the entire house. There are point-of-use humidifiers, which can be small enough to only humidity a single room or your immediate area. or can be large enough to humidity a whole-house by connecting to the furnace.
The most common humidifier, an “evaporative”, “cool mist”, or “wick
humidifier”, consists of just a few basic parts: a reservoir, wick and
fan. The other types of household humidifiers are the vaporizer,
impeller, and ultrasonic humidifiers.
Unnecessary or overuse of a humidifier can raise the relative humidity to high levels, promoting the growth of dust mites and mold. A relative humidity of 30% to 50% is recommended for most homes.
More information and photos of household humidifiers can be found at: http://en.wikipedia.org/wiki/Humidifier
http://www.walmart.com/cp/Humidifiers/133042
http://www.amazon.com/Humidifiers-Home-Appliances/b?ie=UTF8&node=267555011
2. The personal medical humidifier is used with a mask to directly humidify the air that we breathe. This can be a small portable device or a larger one that is supplied by a medical equipment company. Humidification is provided to keep secretions thin and to avoid mucus plugs.
Equipment
Air compressor
Nebulizer bottle
Aerosol tubing
Trach mask
Sterile water
Attach a mist collar (trach mask) with aerosol tubing over the trach with the other end of tubing attached to the nebulizer bottle and air compressor. Sterile water goes into the nebulizer bottle (do not overfill, note line guide). The trach mask should always be above the collection bag and the hose routed so condensing moisture in the hose flows back into the bag and not into the airway. A gurgling sound indicates moisture is collecting in the hose and should be cleared. Oxygen can also be delivered via the mist collar if needed. Proper care and use should be followed per the instructions of your doctor or respiratory therapist.
HUMIDIFIERS – RECOMMENDATIONS
1] Wal-Mart has a good ultra-sonic that holds about a gallon and a half. The output is adjustable so you can add more or less as you need. Radio Shack has a Digital Thermo-Hygro gauge that tells you the temp and Humidity on the same face. It’s battery powered and the batteries last a long time. I can’t remember what I paid for the humidifier or the gauge but both were less than $50 together. I have had mine about 2 years and both work great.
Joe W. – FL
2] I recently purchased a Venta air washer and humidifier. We got the 360 sq. ft. model LW24 to run in the bedroom. It works great and it also cleans the air. We don’t have an instrument to measure the amount of humidity in the room, but my husband has no problems with excess mucus or crusting. We live in Florida where the humidity is generally pretty high except in winter. We have no problems with humidity/moisture build up in the room. PLUS it is very quiet. You won’t notice it is even on. The nice thing about the Venta is you don’t have any filters to replace and it is also almost maintenance free. Every 10-14 days, rinse off the barrel and add some cleaning solution (sold by Venta) that keeps everything clean and mold/mildew free. We add about 1/2 to 1 gallon of water every day (depending on how long we run it). They are not cheap. I think we paid about $300. We are now considering purchasing the larger model that will wash and humidify up to 760 sq. ft. to put in our living/kitchen area. Their website is http://www.venta-airwasher.com/. I purchased mine from Bed Bath and Beyond.
Debbie W. – FL 0207
3] I am 3 yrs. out of surgery, and I have always had a problem with my stoma bleeding during the winter months when I have to use my central heat, and summer months when I use my air conditioner. The culprit, I have found, is humidity, or the lack of it. It is my experience that trying to humidify an entire house is really a chore, not to mention expensive. Instead, I use a personal heat and humidity system. I have the DeVilbiss 8650D aerosol compressor with a trach mask that I sleep with directly over my stoma. The drawback to this setup is the noise the compressor makes. It’s not as noisy as a large compressor, but it does put out a pretty good hummmmmm. But then, you don’t have to use it at night. You can use it during the day while you are relaxing, watching TV, or whatever. Being an old Vietnam Vet, I can sleep through a nuclear attack if I choose to, so the noise doesn’t bother me at all.
If you’ve never seen this setup, it’s a small air compressor with a heated nebulizer bottle attached that you fill with distilled water. Attached to this is a 4 or 5 ft.. length of corrugated tubing with a trach mask on the end. The trach mask goes directly over your stoma with an elastic strap around your neck to hold it in place, and the compressor blows a very light stream of moist, heated air which you breathe. You can do this for any length of time you choose. I personally use mine at night for 7 or 8 hours. When I make my run to the bathroom I refill my water bottle This has completely eliminated my stoma bleeding problem. Sometimes I go days without using it, when I notice a little blood in my mucous I know it’s time to spend a couple nights on my humidifier.
I don’t have a clue to the price of this humidifier, being that it is supplied by the VA. The best I could come up with is an address for the manufacturer:
Sunrise Medical
100 DeVilbiss Dr.
Somerset, Pa. 15501-2125
Of course you will want to see your ENT doctor first to make sure your bleeding isn’t being caused by something else.
Robert P. – GA 0106
4] I have been told the “wicking” type is the most effective and have several of them. They have a large filter in them which the water is pumped over the top and down a sort of channel that causes a waterfall over the top of the filter keeping it constantly wet and the fan blows through the filter evaporating the water. The brand I use is Lasco as it is common in my area and filters and such are readily available. It has a 3 speed fan and a humidistat adjustment on it so you can set it to go on and off when you reach a satisfactory level of humidity and it will maintain this degree of humidity automatically. Mine is a Lasco model 1128 9 gallon recirculating humidifier. It holds about 4 gallons of water and is rated at 9 gallon discharge per 24 hours. I think the cost on this was about $60.00, and I use just this one unit in a very large 9 room old farm house built in 1864. I change my filter yearly unless I have a lot of mineral deposits that don’t clean off then maybe twice a year. I live in the country with my own well and, even with a water conditioner, we have a lot of minerals in our water. But rather than used distilled water I just use a humidifier water conditioner. It cost about $2.00 per quart and mixes @ 1 tablespoon per 1 and 1/2 gallon of water for my situation anyway. I take my filter out usually every two weeks and soak it in warm water then rinse it several times and this removes all the mineral deposits. The most important thing I have found is to make sure you have a humidistat gauge before you start messing with the humidity in your home. If you don’t know what the current humidity is, it will be impossible to adjust it so you are comfortable. You can purchase these for anywhere from $7.00 to $15.00 in my area anyway. Wal-Mart carries them around here and I keep one on each level of my house, one in both my offices and one in my vehicle when I travel on trips as the A/C removes humidity and by shutting it off for several minutes you can bring the level back up again. I have found that every year since my lary operation I tolerate a little less humidity then I did the previous year. I think our bodies tend to adjust to some of our adverse conditions over time.
Wild Bill from MN 1206
Another source for humidifiers and air purifiers can be found at:
https://www.allergybuyersclub.com/
Michael Ricci Class of 2015
CPAP Machines
It has been suggested to use a CPAP machine to provide air and humidity. Caution with the use of a CPAP machine as this can damage your lungs! The pressure has to be set low by a professional that knows how to change the settings. If not set correctly there is a danger of causing excessive pressure resulting in a damage to the lungs. Also they need regular cleaning. The hose and mask need to be replaced regularly. There is also a new machine on the market that cleans the CPAP machine called SoClean.
Ron M. WA
CLEANING HUMIDIFIERS
I have been reading all the postings about humidity and the white dust. I worked in the water industry for 22 years, so this may help. City treated water contains lime, salt or calcium to help soften the water. Home softeners also condition with salt or calcium. When the water is atomized and dries the dust is either lime, salt, or calcium. The use of distilled water (while expensive) will stop the white dust.
George C. – NJ
SUCTION MACHINES
SUCTIONING
It is preferred if you can cough up the mucus or an obstruction. Irrigation with saline solution helps to cough and often eliminates the need for using a suction catheter . Suctioning should only be done by the advice and instruction of the doctor, nurse, or respiratory therapist.
There are many types of suction machines from portable battery units to home based units. It is not practical to cover the machines here. We can however give the basics.
Clearing the airway is important to prevent a mucus plug from blocking the airway and stopping the patient’s breathing. Suctioning should be considered if the airway can not be cleared by coughing. There is always the possibility of damage to the tissues of the airways when a catheter is inserted, so care must be taken. The use of saline solution or the pink water bullets can help loosen and soften mucus, allowing it to be removed easier. If the patient feels or hears mucus rattling in the airway, try irrigation to get it up and coughed out. This is most often needed in the morning when the patient first wakes up. When there is an increased respiratory rate (working hard to breathe), you might need to clear the airways, but if there is a wheezing sound, it is more likely to be needed immediately.
Secretions should be white or clear. If they start to change color, (e.g.dark yellow, brown or green) this may be a sign of infection and you should talk with your doctor.
Clean your equipment, tubing and suction catheter before putting away and before using and be sure your Suction Machine is in working order. Wash your hands before and after handling:
1. Turn on the suction machine and connect the suction connection tubing to the machine.
2. Use a clean suction catheter when suctioning. Whenever the suction catheter is to be reused, it can be cleaned by placing the catheter in a container of distilled/sterile water and apply suction for approximately 30 seconds to clear secretions from the inside. Next, rinse the catheter with running water for a few minutes then soak in a solution of one part vinegar and one part distilled/sterile water for 15 minutes. Stir the solution frequently. Rinse the catheters in cool water and air-dry. Allow the catheters to dry in a clear container. Do not reuse catheters if they become stiff or cracked.
3. Connect the catheter to the suction connection tubing.
4. Suction a small amount of distilled/sterile water with the suction catheter to clear any residual debris/secretions. The collection cup should also be cleaned regularly to prevent bacteria growth and odors.
There are several models of suction machines on the market. The DeVilbiss Vacu-Aide Compact Portable Suction Aspirator Machine 7310PR-D is a great little suction machine. It is smaller than the Drive product supplied by Apria. The little one works great, has all the connections for use in a car, and is lightweight. The only drawback is that it is noisy.
There is another suction machine that is a little bigger and heavier but cost less.The DeVilbiss Portable Suction Aspirator Machine w/ Rechargeable Battery 7305P-D
The cost is around $300 depending on where you purchase them. Most insurances will cover the cost is prescribed by your doctor or home heathcare.
We will not give you instructions for the
actual suctioning because, done improperly, it can cause damage. Your
medical personnel should advise you on this.
For Those With Tracheostomies
Detailed Care information
Do not be confused between Tracheostomy and Laryngectomy. While the hints for cleaning are excellent, Total Laryngectomees use different equipment to insert and are total “neck breathers”. For more information about that and other subjects, you may learn more in our educational videos at:
https://www.drugs.com/cg/tracheostomy-care-discharge-care.html
HME (Heat Moisture Exchange)
Any good stoma cover or filter will act to some extent as an “artificial nose” – will warm and humidify incoming air by absorbing exhaled moisture, which the next incoming breath passes through before entering the stoma and then lungs. The difference in the devices that have been named and accepted by Medicare as “HMEs” is that they seal all around the stoma, so that ALL incoming air must pass through them – none can get in around the bottom or sides – and thus they are often more effective – but not necessarily so. For instance, a Buchanan Stoma Protector, tied snugly around the neck and tucked under the shirt collar, will do a very, very good job of heat-moisture exchanging – not as perfect and complete as an HME, but much, much better than nothing – and as much as a lot of people want or need, especially for the price. Even one of the foam filters under a cotton turtle neck or mock turtle neck will do a pretty good job, as will many of the other types/brands of stoma covers/filters.
Another thing the HMEs do is to force the lungs to work harder to breathe in and out – more like they had to when they had to bring in the air over the tissues of the nose. Again, good stoma covers/filters will do this too – but, again, not quite so completely since they don’t seal around the stoma.
Dorothy Lennox
Total Laryngectomee Rehabilitation and HMEs
You can get more information and reach the vendors in our Suppliers Section.
Benefits of Using an HME – Video
A short video explaining in simple terms and graphics the use of an HME
https://www.youtube.com/watch?v=Q-tETbEkNZ4
The Use of HMEs – A Literature Review (pdf)
Videos demonstrating application, removal and use of adhesive for:
Provox®StabiliBase™ adhesive base plate
http://www.youtube.com/watch?v=jIqu40RWkHQ&list=UUtTiTi3t55jJ4Dr-zNLjBYg&index=3
http://www.youtube.com/watch?v=ayAiqPyYHT4&list=UUtTiTi3t55jJ4Dr-zNLjBYg&index=5
http://www.youtube.com/watch?v=FeostnGjF7A&list=UUtTiTi3t55jJ4Dr-zNLjBYg&index=22
Videos demonstrating LaryTube placement and LaryClips for:
Provox® LaryTube™
http://www.youtube.com/watch?v=Emj2P1YvNbs&list=UUtTiTi3t55jJ4Dr-zNLjBYg&index=8
http://www.youtube.com/watch?v=1TJLXyabeb8&list=UUtTiTi3t55jJ4Dr-zNLjBYg&index=9
Reports from our members
Using with Lary Tube Holder
I wear a lary tube and HME held in place by a lary tube holder worn around my neck. I don’t care for having to stick adhesive things to my throat. I wear this arrangement 24/7 and can go for days with the same HME filter and no cleaning required. My mucus is minimal and I feel very secure and confident in knowing that the air I breathe is pretty much contaminate free. The tube holder and HME are both flesh colored so they don’t stand out. My breathing is always good. If I have to cough, I quickly pluck the filter out of the tube and cough into a handkerchief. I am very pleased with this arrangement and consider it far superior to any other arrangement. But, as you know, we are all different. This is what works for me.
Hank Luniewski
I cut the neck band to about 3 inches on each side and taped each side to my skin . I couldn’t tolerate the constant slipping the band did . It worked a lot like the button clips and it’s free , lol.
Beth Herndon posted this on WWFB 7/19
Early Use of HME
I had my surgery in September 2008, and by November, after the first
successful placement of a prosthesis, I started experimenting with
base plates and HMEs for use. One thing I determined early was I was not
going to use a base plate which I had to glue on myself, so I think over a
two month period, I wore every self adhesive base plate sold by Provox and
In Health. Early on I began leaning toward the Provox products primarily
because In Health was not promoting 24 hour use, while the Provox products encouraged it. Also, it seemed to me the Provox base plates were more secure, or to put it another way, they seemed to stay on my neck longer than the In Health products did.
By January 2009, I was using the Provox Xtrabase base plate due to its rigid
center which accommodates stomas which were somewhat dented in, which mine is. The Xtrabase is also the base plate of choice if using a hands free device, whether it be In Health’s version or Provox’s, as they both fit
onto all the base plates. I never could master the use of the hands free
however, as it made my neck muscles hurt. So, even though I used a normal HME with this base plate, I have been quite satisfied with its service.
I usually will wear an Xtrabase base plate for 48 hours before removing and
discarding it. Also, I am beginning my 4th year of wearing this self
adhesive base plate, and I have never used any other chemicals to aid in
keeping it attached or in help of removing it. One base plate will be used
for 2 showers, with the aid of the Provox shower attachment. Usually,
during the second shower, after I am completed with the shower, I will
remove the base plate and shower attachment and clean around my stoma with the hot spray in the shower. If you do this, you must remember to stand back and not let any direct spray of water into your stoma…if you do
you’ll know immediately. But doing this it really soothes the skin around
the stoma where the adhesive from the base plate was. I think this is the
one primary reason I have not had any significant skin irritations since
wearing the base plates. After getting out of the shower, I attach a new
base plate after cleaning in and around my stoma area and then attach a new HME, then shave, then I am ready to wear this base plate for the next 48 hours.
Of course, during times of infections which cause mucus buildup and more
coughing, I may not be able to get 48 hours out of a base plate, requiring
an earlier change. But looking back over the past 4 years, I can say that
I have averaged 48 hours for a base plate.
Some of the most significant advantages of wearing a base plate and HME is
it is more sanitary. My wife says I have become somewhat “germophobic”
since my surgery, and while I don’t agree totally with that assessment, I
will say how much more important it is is for laryngectomees to practice
good personal hygiene because we have lost the services of what our nose
and nasal cavity did for us, and if for no other reason that the stoma
opening goes directly to the lungs, we should be aware of what we are doing in that area. Early on I wanted to use the HME because I was not having good success getting a good fit when occluding over the foam covering I was wearing, and I would catch myself sliding my thumb under the foam cover to get a good seal on the stoma. By doing that, I just transferred anything I had on my thumb into my lungs, which is not good. The use of the HME eliminated that concern, and for me, made it easier to talk because when using the HME, you will always get a 100% seal when pushing the HME down.
Another advantage is the chemical which is in the foam filter in both brand
HMEs will, for most laryngectomees, reduce the amount of mucus your body will produce, which will then reduce the amount of coughing. The key word in this saying is most. It worked exactly that way for me (after about 2
full months of use). However, it will not work this way for everyone. As
we have heard over and over again, and it is very true, we are all a bit
different in the amount of tissue we had removed, the amount of cancer we had, our overall health, our ages…..I could just go on and on with
reasons why we are all different somewhat, which only means our outcomes from using various products will almost always be somewhat different.
My biggest advantage of using a base plate and HME is that it gave me an
extra level of protection when I am out in the public. It’s an extra
expense and it creates a bit more work, but the use of these two products,
along with the silicone prosthesis, gets me closer, in my mind, back to the
feeling of being normal. My stoma is located low enough on my neck so
that when wearing a base plate and HME they can be concealed under clothing, which just gives me a better sense of normalcy. I can easily wear a shirt and tie while wearing the base plate and HME, which is just another plus for me.
I hope this has helped explain at least my use of the base plates and the
HMEs, and maybe assist those who may be considering using them or wondering what they were.
Mike Smith
9-11-2008
Using a Lary Tube to allow skin to heal
You can cut the lary tube strap ends off at approx 3 inches. Clip them on your lary tube and use some surgical tape to hold the strap ends to your skin. I did this for almost a year waiting for my skin to heal enough so I could use adhesive baseplates.
Rita Burfitt
Filtering effects of HMEs – Woodwork
I was working on an old bench this morning that I am modifying to put in my kitchen. I was removing the old leather seat and back and the rock wool and straw stuffing that was used for padding. I also did some scraping and some sanding. The wood is black walnut.
I was wearing my HME filter and decided to take some comparison photos for folks to see that show the filtering that the HME provides.
One photo is of the old bench.
There are two (front & back views) showing the dirty HME beside a clean/unused HME One photo shows the dirty one torn apart.
My standard procedure is:
I use one of the bib type filter with open web type material and a foam filter inside. I dampen it and put it on over my HME. It catches a lot of stuff and keeps the HME a LOT cleaner. Sometimes I take a big bandana style kerchief and fold it diagonally, dampen it, and tie it around my neck over top of the HME I did not do that the day I took the photos. I was just wearing the HME filter.


Bruce Buck Martin
Use Clip to hold Lary Button
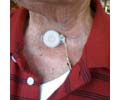
Alligator clip is used to hold the Lary button and is great for hands free.
When I cough the cap sometimes goes flying so I anchor it with a clip to attach it to my clothing.
Paul Frehner 2009
HMEs


Heat/Moisture Exchange (HME) filters are a type of stoma cover which help laryngectomees partially restore functions previously performed by our noses and upper airways. They might be thought of as “artificial noses.” As the name implies, an ?exchange? of heat and moisture occurs in the HME filter as a laryngectomee inhales and exhales. During exhalation, warmth and humidity are conveyed from the lungs and deposited into the filter. During inhalation, the warmth and moisture are picked back up by incoming air and returned to the lungs.
HMEs are receiving more attention in the U.S. as the results of research which has been conducted in several European countries becomes more widely known, and certainly because they are now covered by Medicare.
Before the laryngectomy, the upper half of the breathing system filtered, humidified and warmed incoming air. It also provided resistance so that the lungs fully inflated. This helped maintain lung capacity, and facilitated an efficient exchange of gasses in the lungs (oxygen added to the blood stream and carbon dioxide removed). Prior to the laryngectomy, by the time the inhaled air reached the lungs it was saturated with moisture and its temperature was close to the body temperature of 98 degrees Fahrenheit (37 Celsius). Air at 100% relative humidity and 98 degrees is ideal for oxygen/carbon dioxide gas exchange. After the laryngectomy, the incoming air was dirtier, drier and cooler.
The resistance function of the nose and upper airway might be a little more difficult to understand than dirtier, drier and cooler air and the problems those produce for laryngectomees.
Prior to the laryngectomy, the nose provided 80% of the resistance to breathing; with the mouth, larynx and trachea providing the rest. By providing resistance the lungs had to move air a further distance, and past curved and sticky mucus covered surfaces which resisted the air flow. This consequently made us “work” harder to breathe. We had to breathe more deeply to move the amount of air we needed. This helped maintain lung capacity (the volume of air our lungs could hold), and the efficiency of the gas exchange in the lungs where oxygen is added to the blood stream and carbon dioxide is removed. The quantity of oxygen in the blood of laryngectomees is measurably reduced if they do not compensate for the loss of resistance. And our breathing efficiency typically declines, particularly in the months immediately following the surgery.
All laryngectomees can use an HME regardless of their method of speech. There are basically two different types of HMEs, and two major ways to attach them to the stoma. One HME type is designed for TEP prosthesis speakers who cover their stomas (occlude) with a finger or thumb in order to speak. This same type filter can be used by traditional esophageal speakers or those who use ALs (artificial larynges). It consists of a housing and a filter.
A second type of HME is for TEP prosthesis speakers. It combines the HME filter with a hands-free valve. The hands-free valve closes when the TEP prosthesis user exhales, and air is redirected into the prosthesis without having to cover the stoma with a finger or thumb (hence the term ?hands-free?).
There are two basic ways to attach an HME or HME/hands-free valve combination. In one, the housing is glued to the skin around the stoma, and the HME snaps into the circular hole in middle of the housing.
Some systems have reusable housings and the user applies the glue in liquid form to the housing and then lets it dry. Other housings are pre-glued and are disposable after using them for a day or two.
In either case, the skin surface around the stoma is first cleaned in order to get good adhesion. Many use rubbing alcohol for this purpose. Some of those with sensitive skin also use a product such as ?Skin Prep? or ?Skin Shield? as a barrier between their skin and the housing glue. Several suppliers have pre-glued disposable housings which use special formula glue for those with sensitive skin.
A second method for using an HME filter is to combine it with a laryngectomee tube (vent, button). Two laryngectomee tubes/vents/buttons which are designed to accommodate an HME filter are the Lary Tube from ATOS, and the Barton-Mayo Button from Bivona and InHealth. The Trachi-Naze Plus system combines a lary tube with a finger occluded HME. Both the ATOS Provox filter cassette HME and the InHealth Blom-Singer HME fit into these tubes.
In addition to helping maintain the cleanliness, temperature, humidity and resistance to the air we breathe, HMEs have other benefits. In addition to mucus reduction, another of the most important of these is that many laryngectomees who speak via the TEP (tracheo-esophageal puncture) prosthesis report that their voicing is improved through the use of the finger occluded HME or the hands-free valve/HME combination. In the case of the finger occluded ones, it takes less pressure to get a good seal around the stoma to get a good and loud enough voice, and less pressure is applied to the entire area. This often results in speech being easier to produce as well as more clear to your listener.
Heat/moisture exchange filters (HMEs) need to be tried for a period of time. Using them continuously for at least one week is the minimum time they should be tried. The reason is that unless you just had your laryngectomy, you have gotten used to the lack of resistance to air moving in and out of your stoma. You may find the initial experience a little unpleasant and feel that the HME is restricting airflow. It is, but in beneficial ways. It takes time to get past this sensation and for you to adjust to it.
But in addition to this feeling, it also takes time for the HMEs to demonstrate some of their most important benefits such as reduced coughing and mucus production. And these benefits are unlikely to become obvious to you for a week, or even longer. A major mistake would be to try them for a day or less and conclude that they restrict your airflow. Research has shown that laryngectomees are more likely to stick with the use of HMEs if they are introduced right after the laryngectomy. The longer we go without using anything which provides resistance the more difficult it becomes to stick with them. We have simply gotten used to less restricted airflow and the sensation of having to work harder to get air is felt by many to be uncomfortable until they have adjusted to it.
Those with breathing problems such as COPD (Chronic Obstructive Pulmonary Disease), emphysema, asthma, etc., should not try an HME without approval from your MD. But trying them has been made easy since the major HME producers will send you a free sample kit of their HMEs (but not the hands-free valve/HME combinations) upon request.
If you wish to try them, you might consider trying those which have the least resistance first, and then move to those with greater resistance. This would suggest trying the Blom-Singer (or ATOS HiFlo cassette) first, and then to the ATOS Regular cassette, and finally to the Kapitex filters. The Kapitex nighttime filter provides the greatest resistance, so it should probably be tried last after you have gotten used to the feeling of added resistance to air flow, and it should only be used during sleep.

HMEs cannot completely restore the functions of the nose and upper airway in conditioning the air we breathe to the standards we enjoyed prior to becoming laryngectomees. They can, however, make a significant different in reducing coughing and excessive mucus production, and deliver a better quality of air to our lungs than the alternative stoma covers. They can also make a noticeable improvement in voicing for many, and they can help maintain lung function. While some laryngectomees will decide that they are not worth the additional hassle of using them or their cost, every laryngectomee should at least consider giving them a fair trial.
Hints from members on wearing base plates for HMEs
1. When I am working at a client site, I use the prep and remove wipes, but
when I am at home, I simply use the base plate without any additional prep.
One suggestion I have for those who don’t like/can’t use the adhesives and
removers is to warm the base plate’s own adhesive with a hair dryer prior to attaching to the skin. I put the base plate on the countertop, adhesive-side up, and run a handheld blow dryer over it for 15-20 seconds. This makes the adhesive softer and it adheres to the skin with much better results than when I try to warm it up by hand as the instructions state.
When I know I am going to be speaking a lot during the upcoming day, I will
combine both the hairdryer and adhesive approaches and I get a really
durable seal. This has been helpful for those interminable status
meetings, conference calls, training sessions, etc.
Just a hint I picked up at the IAL convention a few years back…..
Loyd Enochs
2. I use Provox Flexiderm bases and when I started using them I used Skin Prep and Skin Tac but soon found I was allergic to them so I use only the base and the built in adhesive. However I do not use a hands-free.
Charles Rickard
3. I used Skin Prep & Skin Tac for a couple years when applying my base plate and had problems. The base plate would last maybe two days and I also had the itchy skin rash trouble. So, I stopped using the other adhesives and now just use the base plate by itself. And, to combat the skin problems, I now apply skin oil to the area the night before putting on a new base plate in the morning. Skin oil is used to help healing scars after an operation, so I figured I’d try it around the stoma – and it really has cured my skin rash troubles. You might think any oil would cause a problem with getting a good seal. But most of it sinks into the skin and the rest washes off easily.
Also, I was instructed by my SLP to clean the area with an alcohol swab. But, I then realized that it doesn’t make any sense to put alcohol on skin that already has a rash. Now I just clean the area using a neutral pH soap that doesn’t have any oils in it. I now get 4-6 days on a base plate, with no itchy rash — and I talk a lot! Hope this helps.
Pete Meuleveld
4. My surgeon is great; the man undoubtedly saved my life after chemo and radiation didn’t quite do the trick. So, my family, friends, and I adore him. However, my experience so far suggests that skin problems, issues with base plates, and prosthesis in general are best addressed with your SLP vs. the doctor. I’m no expert but these are my thoughts.
Generally, the aloe wipes help me with skin irritation. Occasionally, I’ll get a spot that is particularly irritated. There I use Neosporin (on the outside only) with pain med for an hour or two, without a base plate. This helps a bunch, especially if there is an actual break in the skin.
Tom Whitworth
Alternative With Physical Activity
I am an outdoor activity enthusiast, walk/jogging, biking, hiking, and backpacking, so I am very concerned about protecting my stoma from anything but air being inhaled. I don’t have a voice prosthesis, which makes protecting my stoma less complicated. You are probably aware that the ways mosquitoes home in on us, as a food source, is their acute ability to detect carbon dioxide, doer, temperature, and movement, so we are prime to go items on their menus when we are out rock’in and roll’in. I used the HME base plate filter system at first, when I was able to get back into action, but I too found them very frustrating and unsatisfactory, because I was always blowing them out with my heavy breathing and sweating. I just happened to have some Humidi-Foam Stoma Filters which I had received a sample of from Bruce Medical Supply at one of the Annual IAL Meeting/Voice Institutes, so I decided to give one a try for a walk/jog, and was delighted to find that it stayed in place without a problem. I do, however, also utilize an UnderArmour (my preferred brand) “compression” shirt, under my usual activity shirt (always made of a technical microfiber material), to hold it securely in place. The reliability of the foam filter was a fabulous discovery for me, and I find that there have only been a few times when the filter adhesive has failed during the past few years and multitude of heavy breathing, sweaty actives for which they have worked without a hitch. I keep a bandana handy in case I am caught in dusty conditions to add an additional layer of filtering.
Tucking the bottom of the bandana into my compression shirt keeps it securely in place. The compression shirt also has the property of wicking moisture away for quicker evaporation, and thus works to help cool the body. Have a great time on your outdoor adventures. I’ll be doing a combination bike/hike in the wilds of central Florida this weekend which I am very much looking forward to. Happy trails!
Patrick Kerr Class of 6/11
Here is a study comparing the use of moistened stoma covers with commercially produced HMEs. This can be an option with heavy exercise.
https://www.ncbi.nlm.nih.gov/pubmed/25728911
Working in Areas with Fine Dust
When working around fine dust, I find that a damp cover over my stoma helps a lot. I often also use the ATOS micron filter, which does a great job. I also wear the micron filter when I am flying. When working in dusty environments, I check the inside of the filter. If it is dirty then the dirt is getting into my lungs and I need to do something differently to protect myself.

Ron Mattoon Seattle 2010
posted 10/2019
FREE HME SAMPLES
Just call these toll free numbers (or e-mail or write the companies) and request their free HME sample kits.
Do not know if these are still offered but, if not, they can send a catalog or literature.
ATOS
Six self-adhesive baseplates (round and oval regular, FlexiDerm and OptiDerm adhesive), ten Provox HME cassettes (five normal and five HiFlow), Two Remove adhesive remover wipes, “Life as a Laryngectomee” brochure.
Atos Medical, Inc.
800-217-0025
Fax: 414-227-9033
Email: info.us@atosmedical.com
2202 N. Bartlett Ave.
Milwaukee, WI 53202-1009
InHealth
One reusable humidifilter holder, seven foam filters, five TruSeal adhesive disposable housings, and a guide book. You get a one year membership in Medic Alert by requesting the kit.
InHealth
800-477-5969
Fax: 805-684-8594
Email: order@inheallth.com
1110 Mark Ave.
Covers and Patterns
Wear one. These come in all shapes and sizes, are made of different materials and are offered by most suppliers. A good weave is something that the air can easily get through but a fine enough weave to filter. They can be plain cloth or foam squares, turtlenecks, crocheted collars, or made of a bandanna or a scarf. They come in different colors and sizes, can be purchased or homemade. The benefits are many to you, the laryngectomee, and others will appreciate the “cover up”.

EXTRA STOMA COVERS
All it takes to mess up a stoma cover is one unexpected sneeze or cough. Keep extra foam stoma protectors in your glove compartment as well as in your desk or locker at work.
NO STRINGS TO TIE
If you are sick of tying the strings on
your stoma cover, journey down to your local fabric store and purchase a
few small cord stops. these normally will sell from $0.25 to about
$1.00 depending on style and quality. You can even color coordinate them
to your stoma cover or get the clear ones and they will match any
color. I would advise staying away from the cheap ones that use a hollow
moving stem as they tend to fray the stoma cover strings much easier
than the solid plastic stems. This has worked for me for over 4 years
now and I just leave them on the stoma covers permanently and launder
the covers by hand with the cord stop intact. (Wild Bill from Minnesota)


Stoma Covers with Dirty Environments
When in dirty environments as in working under my car or riding my quad in the mountains, I wear and moistened cover over my HME to catch a lot of the dirt and dust so it does not plug my HME so quickly. It can be a cloth or crocheted one as long as it is easy to breathe through. It can even help when mowing your lawn.
Ron Mattoon Seattle 2010
Posted 2017
HOW I LEARNED ABOUT STOMA COVERS (for women)
When I became a laryngectomy, it was very nice that the hospital gave me a couple of crocheted “bibs”, made by volunteers, to wear over my stoma. My mother took over crocheting of these bibs for me. When I returned to work, I wore either a bib or turtleneck tops (long sleeve in the winter, short sleeve in the summer).
I joined our local support group but most of the members were men with just one or two other women, so I didn’t get a lot of advice about clothing.
Then one of my daughters was going to get married. I didn’t want to wear a bib or a turtle neck for my daughter’s December wedding. So I planned to make my dress but I enlisted the help of women from WebWhispers. I said I’d make a high necked dress—WRONG—I was told the neck had to be BELOW the stoma in case I needed to cough and clear the stoma. The material of my dress would not be stretchy and pull out like a turtleneck sweater. Someone then suggested that I wear a scarf to compliment the dress, but to cover the stoma. I argued that I wouldn’t be able to breath with a scarf of a silky type of material. WW women told me to wear one of those foam covers under my scarf to prevent the scarf from sucking up into the stoma as I breathed. Problem solved.
Then I saw that the IAL was going to meet near Chicago (we live in Milwaukee, WI). So my husband and I went. I knew they would have some dress-up dinners and a dance where, hopefully, I’d see how other laryngectomy women dressed for nicer occasions. WOW. Do they know how to DRESS UP. Very fashionable scarves, beaded necklaces large enough to cover the stoma, fancy “bibs” of lace or needlework, necklaces that look like a large brooch covering the stoma. And their dresses were anywhere from just below the stoma to considerably lower–definitely not all turtlenecks or plain bibs.
When we went on a cruise with WebWhispers, the dressing-up got even better with the Captain’s Dinners. This time I was prepared.
WebWhispers has several venders who sell these fancier bibs and necklaces. I bought my necklace from one of our members who was listed in our Webbies Workshop. She was in Chicago at the IAL, sized a necklace on me and we determined that she’d have to make it a bit smaller as my neck is very thin. If I need to cough, I just go to the bathroom, turn my necklace around on my neck, and do my coughing and cleaning.
I’ve gotten so many compliments on my necklace.
Vicki Metz
Check Out Our Webbies Workshop
For gorgeous custom designed beaded stoma covers and beautiful crocheted scarves and covers, please take a look at the photos in this section. Yes, they are for sale. Info in the suppliers section.
Many of our WebWhispers Suppliers also handle beautiful stoma covers that add something extra to your costume. Check out their catalogs.
METHODS TO TIE SCARVES
Whether you elect to tie, pin or wear your scarves loosely, you can make a fashion statement and feel comfortable about wearing your scarf.
Ways to Tie a Scarf
Video. Had commercial first, then in less than 5 minutes shows you 25 ways to tie a scarf:
A section of our site with several ideas on neck coverings refer to the Suppliers section.
PATTERNS FOR STOMA COVERS
Laryngectomy Covers (Stoma Covers)
These first two were sent by the wife of a WW member laryngectomee:
Materials: Crochet Cotton – Size 10
Steel Crochet Hook – Size 2
Original Pattern
1. Chain 5″ (Approximately 35 stitches)
2. Single Crochet in 2nd chain from hook and continue across chain.
3. Chain 2 and turn
4. Double crochet across row, repeat rows until 5″ is reached
5. Chain 3 and turn.
6. Triple crochet in next 5 sts.
7. Double crochet across row until last 5 sts.
8. Triple crochet in those last 5 sts.
(End of Bib)
9. Chain 50 sts. then single crochet back until end of row.
10. Chain 50 sts. Again for another tie, single crochet across chain, back to bib, and tie off.
My husband found the stoma covers to generally be too small. He has a large neck size and wanted a larger bib, as well as longer ties. Also, due to the necessity of frequent laundering of the stoma covers, we found that the ties had a tendency to break down faster then the bib itself. Rather than throwing away the entire bib, we opted to make the bib separate from the tie. This way, we can remove the tie when it breaks and replace it with a new one. He also feels that this version fits a little better and is more comfortable.
Alternative Pattern for large neck
(Neck Size 16 1/2 – 18)
Approximate Finished Size – 5″ High by 7″ Wide.
1. Chain 45 stitches
2. Single Crochet in 2nd chain from hook and continue across chain.
3. Chain 2 and turn
4. Double crochet 18 to 20 rows depending on preference.
5. Chain 3 and turn.
6. Triple crochet in next 8 sts.
7. Double crochet across row until last 8 sts.
8. Triple crochet in those last 8 sts., and tie off.
Ties – Chain until you reach a length that circles the neck comfortably with ample length for tying. Then single crochet back across chain and tie off.
Weave the tie in and out of stitches in top row of bib. This gives a slightly gathered effect, which aids in holding the bib away from direct contact with the stoma.
A Simple Pattern for a Crocheted Stoma Cover
Since the covers can vary in size considerably and one person might like more coverage than another, my friend wrote out these very simple instructions for a bib with ties.
You can easily make it whatever size you wish. My favorites are 5″ to 6″ wide and 4″ to 5″ deep.
10″tie_____________[__6″ bib ____]______________10″tie
Instructions for one approx. 6″ wide
Use inches for measurements instead of counting stitches. This allow for variation in thread and hook size as well as the use of different kinds of stitches
Chain 26 inches (for a bib that is 6 inches wide with 10 inch ties) turn, slip-stitch in first10 inches of chain. Triple crochet in each chain for the next 6 inches. Turn, chain one, then triple crochet in each triple crochet. Repeat until bib is as long as you want it: 4, 5,or 6 inches. Single crochet around the outside edge to the single chain (the 10 inch tie you did not slip stitch). Finish off.
Using this last pattern, a crocheter made some for me to see with a size 5 thread (instead of the #10 in the top one) using a Size D needle, and they are great, so experimentation is encouraged! Just got this from her:
NOTE: When tying off and cutting thread, be sure to leave a tail at least 6″ long so you can thread it onto a yarn needle and weave it through the back side.
With size 5 thread and size “D” hook, chain 33.
ROW 1 – Single crochet in second chain from hook and across (32 stitches).
ROW 2 – Chain 2 and turn, DC across.
ROW 3 – Chain 2 and turn. DC, inserting hook between stems and below all horizontal threads connecting stitches.
Continue working same as row 3 until desired length (last DC row should be back side of work.) Chain 1 and turn to right side and work 1 row of sc across. Fasten off.
TIES: Attach thread in top corner of bib. Chain 1, then sc in next stitch. (chain 1 and turn, then sc in next 2 stitches,) until tie is approximately 10″ long. Work other tie in the same manner.

Here one for knitters:
Cast on 3″ worth of stitches in soft cotton and either work in a non-curling stitch such as garter, seed, or moss, or work in stockinette stitch with a garter stitch border. Increase at each end of every other row until 6″ wide and work even until 5″ from beginning. Shape as for the neck of a pullover by working a quarter of the stitches, binding off one half of the stitches, then shaping the final one quarter by decreasing on the neck edge every other row until one stitch remains; then work other side to match. Use I-cord to edge the top and form ties, or even quicker, make a 15″ crocheted chain, continue by working single crochet across the neck edge, and then crochet another 15″ chain. Use these pieces as a way to try out new patterns, either lace, cable, or multi colored. These are for men, women, and children, so use your creativity!
And another sent by a knitter:
CAST ON 2 STS.
WORK IN ANY ST, OF YOUR CHOICE.
INC, 1 ST AT THE BEGINNING OF FIRST AND EVERY ROW,
UNTIL THEIR ARE 56 SSTs.
NEXT ROW.
INC IN FIRST ST, KNIT 11, THEN [KNIT 2 TOG] 5 TIMES.
KNIT 12 [K 2 TOG] 5 TIMES, SHOULD HAVE 47 LEFT.
CAST OFF. MAKE YOUR TIES
Easy knitted stoma bib
Size 7 (US) needle
Worsted weight cotton yarn
Size G crochet hook
With crochet hook, chain 61, place last loop on knitting needle
Use a single strand cast on and cast on 23 stitches (24 total on needle)
knit one row (you’ll be back at the chain edge)
Row 1: Slip first stitch as if to purl, K1, k2tog, knit to last three stitches, k in front and back of next stitch, k2
Row 2: Slip first stich as if to purl, k across
Repeat these two rows five more times.
Work even (slipping the first stitch of each row) knitting each row with no shaping for 24 rows.
37.On next row, slip first st as if to purl, K1, K in front and back of next stitch, K to last four stiches, K2 together, K2
38. Slip first st as if to purl, K across
Repeat 37 and 38 four more times
Repeat row 37,
Bind off in Knit on next row, when one loop remaining on needle, pick it up with crochet hook and chain 61, turn, slip stitch in each chain, single crochet in each row end loop across top of bib, slip stich back up other chain. Knot or weave in ends. No other finishing needed.
Marcie Hanaburgh
Hints from a crocheter
For the crocheted ones you can use any pattern you would use for an afghan and just make a 6″ square. There are books with hundreds of patterns. Even grannies squares or patterns for bibs or coasters, pot holders, etc. They just need to be adjusted a little and of course you can’t use the really open lacy ones.
USE BIAS TAPE FOR TIES
I’ve been making bibs for my grandfather for over 25 years and I just make the bib then sew narrow bias tape ( 10″ ties and the width of the bib) onto it. They hold up for a long time this way
A BLANKET COVER
Use 100% cotton, lightweight thermal baby blanket and bias tape to match blanket.. (One example is “All Season Knit Receiving Blanket” by “Baby Morgan”, 30 x 40 inches, sold at WalMart). Make a pattern for the stoma cover. One possible pattern is about 10 inches tall; 9 inches across the bottom; 7.5 inches across the top. The bottom edge is squared off. The top edge is curved slightly down at the center to fit comfortably at the neck. Wash blanket and using the pattern you have made, cut out stoma covers. Finish the two sides and the bottom edge of the stoma cover with bias tape. Cut a piece of bias tape 3 feet long. Match the center of the tape and the center of the top of the cover. Sew the tape on, leaving the extended ends so they can be tied at the back of the neck. Care should be taken so that no small pieces of thread are left on the finished product. They could be dangerous if inhaled.
Ora Mae Hardin
MAKE A COVER WITH A FOAM LINER
I have been a Lary for 6.3 years and using a TEP for almost 6 years. I had designed a stoma cover using dual layers of thermal knit fabric to give me a semi heat exchanger and stoma cover. About 1 and half years ago I was diagnosed with a second primary on my left lung and decision was made to operate. The operation was done and they had to remove my whole left lung for all to be well with me.
Now I am a Lary with one lung. I thought I might want to protect my single lung a little better than I had been when I had 2 of the things. I had experimented with foam covers and HME’s, but was unable to maintain a useful seal for an extended period of time. I didn’t like the cost of the foam on a daily basis and then I had my insight that has worked for me and others. That insight was to glue the foam to the stoma cover. Simple and very effective. I am able to wash my covers without losing the foam filter and have been doing this since about May of last year with no harmful effects and an incredible reduction in foam filter costs. One other benefit that arose was being able to spritz/mist between the filter and stoma cover to provide added moisture when the humidity is low.
Overall = 11″ , across = 8.5″, bottom to neck opening = 5 or 5.5″ , straps = 1.25″ Foam = 2.5 x 3″ You will want to use double sided clear tape to put the foam on the cover. I use Velcro to close in the rear and I used 1″ x 1″ pieces. Don’t forget that the Velcro go on opposite sides.
Craig Smith

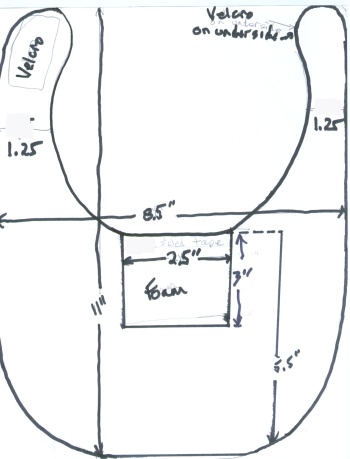
T-SHIRT TO STOMA COVER CONVERSION
(from November 2000 WW Journal)
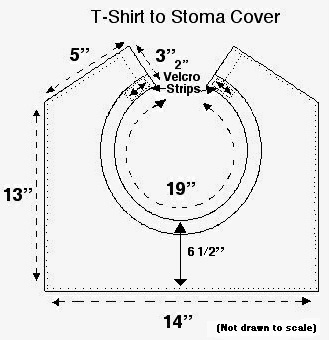
For those with some sewing skills, converting an old favorite (or even new) t-shirt into a stoma cover is not particularly difficult.
The process begins by cutting the collar downwards all the way down the back of the shirt and through the bottom hem. At about 3 inches down from the collar ends, cut the fabric at right angles for a length of about five inches, and again at right angles down the front of the shirt through the bottom hem. Cut the remaining material off at about 6 1/2 inches below the front of the collar at right angles to the vertical cuts.
Fold the cut collar ends over about an inch with the edges on the inside of the shirt. Use a zigzag stitch to sew along the cut edges. Sew a 2 inch strip of velcro, hooks side up, on the outside of the collar end; and a 2 inch strip of the loops part of the velcro on the inside of the other collar end. (You want the hooks side on the outside so it does not irritate the skin.) Finish by sewing the edges of the stoma collar to keep it from fraying.
One prominent SLP noted that anyone who has done laundry before and cleaned out the drier lint filter can attest that cotton and other fabrics shed fibers. There can be quite a few fibers which can come from even a small load of washable cottons. With this in mind, it would be best to wear your homemade cotton stoma cover on top of a foam filter (or HME) to keep fibers out of your stoma.
Still another option to that is to put a partial lining on the reverse side of the cover. For this you should use a porous fabric which does not shed much, if any, such as chiffon-type synthetic fabrics; or the kind of fabric used in bathing suit linings. Just cut a 4 or 5 inch piece of this material (you might double this size and fold it over for additional protection) hem it all around, and sew it to the top on the inside of the cover at the collar hem so that it will be centered over the stoma when worn. It only needs to be sewn at the top edge.
The pattern graphic is not drawn to scale. This pattern shown can also be used to make a stoma cover from scratch. You may also have a favorite stoma cover which you can use as a pattern for making your own. Happy sewing.
THE LEE SCARF ASCOT

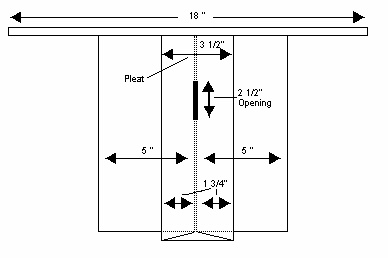
Instructions:
1. Cut a piece of fabric 16? wide and 14? high.
2. Cut a piece for the band 19? long and 3? wide. This step is done at the ironing board. Turn in 1/4? on each end. Fold in half lengthwise, press, and turn in 1/2? on one side. Add some interfacing and press with the iron.
3. Mark the center of the scarf and center of the band.
4. Stitch a small rolled hem on three sides of the scarf.
5. Run a gathering stitch 1/2? from the raw edge. Pull to gather to 9 1/2? in width.
6. With the outside of the band to the inside of the scarf, pin the band to the scarf matching center marks and spread the gathers as evenly as possible. Stitch.
7. Turn the band to the outside of the scarf, turn up the seam allowance on loose ends and stitch.
8. Stitch on velcro: about 3 1/2 inches at the band ends.
To wear it, roll the band under twice, then attach the velcro as tightly or loosely as is comfortable and tuck it down the shirt front.
Note: You can do wider, longer, shorter, or narrower.
For those needing to occlude the stoma with a thumb or finger, use the following: (1) Cut a piece of fabric 25? wide and 14? long. (2) Fold in half. Make a box pleat 1 3/4 deep and 5? from each edge. (3) Make a 2 inch opening 3 1/2? from the top edge and use either a buttonhole or zigzag stitch to keep it from unraveling. (4) Finish using instructions beginning at number 2 above.
Arlene and James Lee
BEETON’S BOOK OF NEEDLEWORK
To download, click here:
Project Gutenberg’s Beeton’s Book of Needlework, by Isabella Beeton
From Samuel Butler’s Preface, writte 1870
INSTRUCTIONS in TATTING, in EMBROIDERY, in CROCHET, in KNITTING and NETTING, in BERLIN WOOL WORK, in POINT LACE, and GUIPURE D’ART are prefixed to the pages devoted to these separate branches of needlework. The whole work is interspersed with coloured and other Patterns in Point Lace, Guipure d’Art, Tatting, Embroidery, and Designs for Monograms and Initials for marking handkerchiefs and table-linen. The quantity of materials required for each class of work is also given with every pattern.
The idea of combining a series of minute and exact instructions in fancy needlework with useful patterns was conceived some years ago by one whose life was devoted to the inculcation of the practical duties of woman’s life, and to assisting her sex in their daily work of HOUSEHOLD MANAGEMENT and REFINEMENT.
Her great wish was that her BOOK OF NEEDLEWORK should be as valuable in its way to her Countrywomen as her work upon Household Management was useful in showing the best mode of providing for the diurnal wants of families. Other hands have brought to a conclusion her original plans. The best attainable workers have contributed to this volume. Only those who knew the extent of the late Mrs. Beeton’s design, will miss, in the pages now before them, “the touch of a vanished hand.”
[This eBook is for the use of anyone anywhere at no cost and with almost no restrictions whatsoever. You may copy it, give it away or re-use it under the terms of the Project Gutenberg License included with this eBook or online at http://www.gutenberg.org]
Mucus Issues
MUCUS – MUCUS – MUCUS
We not only have a problem with thickened mucus in the stoma but often in the oral cavity. We have hints under Post Laryngectomy for humidification and irrigation and under Stoma Care for thinning mucus and what to do about dried mucus in the stoma. However, this surgery or radiation can create very thick saliva and mucus in the mouth and throat. This can make talking, eating, and swallowing difficult. Early after surgery, almost all of us carry water with us everywhere we go. This section will be for suggestions to help us with that continuing situation.
1. SOFTEN DRIED MUCUS FIRST
I found out the hard way that you should first soften dried mucus which can accumulate around your stoma before trying to remove it with tweezers. You can really irritate your skin if you pull dried mucus from the stoma area without first softening and loosening it. If you shower or bathe in the morning, let the water vapor or steam soften dried mucus before removing it with your tweezers. Warm water on a dampened washcloth will also do the trick. For those who have the TEP prosthesis, the tweezers are also handy to use along with a tiny brush and modified hypodermic style syringe/pipet to keep the prosthesis clean.
2. ANOTHER WAY TO SOFTEN DRIED MUCUS
When you first get up in the morning wet your stoma bib. By the time you take a shower, that moisture will have softened the mucus you see, plus loosened some you couldn’t see so you get a productive cough and start the day right. You may not need to use tweezers since thinned mucus coughs or wipes out
3. PICK UP MUCUS WITH TEP BRUSH
I’m sure everyone is familiar with trying to remove wet mucus from around or just inside the stoma, stuff that is not deep enough in the trachea to cough out. Tweezers are fine for dried gunk but, at least in my case, just pulls the wet stuff out in strings, it lets go and springs back. It’s an unending chore. In the meantime I gurgle as I breath. I take the TEP prosthesis brush and roll it around in the wet mucus. It winds up like spaghetti on a fork. Three or four windups and the mucus is gone. I rarely use the tweezers anymore. To make the twirling between my thumb and forefinger easier, I removed the handle from the end of the brush.
Good luck, Bob Power
4. COTTON SWABS
Cotton swabs can be used to clean mucus around the stoma but should NEVER be used inside the stoma. There are two types of cotton swabs and the ones that you should use are the medical type which are longer and have a swab only at one end. These type do not leave lint. The common cotton swabs that you buy at the store are Very dangerous inside the stoma. The tip can come off and go down into the lungs.Caution should be used as they can be harsh on the delicate tissue of the stoma and can cause bleeding, so use they are best used on the outside or entrance of he stoma.
Ron Mattoon Seattle 2010
5. GUAIFENESIN
Used for keeping mucus thin. From the Internet >>>Guaifenesin is an expectorant, a medication that promotes elimination of mucus from the lungs. The expectorant effects of guaifenesin promote elimination of mucus by thinning the mucus and lubricating the irritated respiratory tract. Guaifenesin is an ingredient in many over-the-counter cough and cold products. Guaifenesin was first approved by the FDA in 1952. Some laryngectomees take this on a regular basis and in varying amounts. Most everyone takes it when they have a “cold” in one cough syrup or another. Please take it with enough water to make it effective. It’s purpose of liquefying mucus needs the water and you may find that less medication with water works better than a lot of medication without extra water. Robitussin or Tussin (Most drugstore chains have their own brands, Read the label.), is a non-prescription liquid cough syrup and is 100mg guaifenesin per teaspoon. You want the one that is all guaifenesin, nothing else added. It should be marked something like Robitussin PLAIN, not the CF or DM which have other ingredients. Humibid, Humibid LA, Fenesin and other prescription guaifenesin is in tablet forms. 200mg, 300mg and 600mg. See your doctor. If you can’t swallow the large pills, and they have a 300mg capsule that can be opened and sprinkled…BUT I haven’t been able to find it or order it, so I keep some Plain Robitussin liquid to use if I feel I need some help with thinning mucus. First, I try extra water alone. Surprising how much help that is and how seldom we think of it!
Pat Sanders
6. MORE GUAIFENESIN
Something that I do on occasion when I know that I will be in very dry air, i.e. airplane, long car ride, etc. I take Guaifenesin to help keep things lubricated and thin. It seems to work for me. This way I’m on top of things, a little preventive medication.
Rita Burfitt
7. CLUB SODA USE – Use The Bubbly Kind
My doctor recommended sipping club soda for cutting loose the mucus from the throat and making the mouth and throat feel less dry. He suggested you buy it in small bottles so it doesn’t go flat because the carbonation is part of what works so well.
8. MORE CLUB SODA – Freshening Mouth After Brushing
Way back when…I knew about club soda to help with mucus problems. I do not have a TEP so I can’t gargle. When I brush my teeth, I never really feel fresh, always feeling a residual toothpaste, bubbles, etc., in the back of my mouth and throat. The other day, I remembered the club soda and decided to try rinsing with it after brushing my teeth. Wow! Feel much better. Thought this might be a good tip to add to our list.
Rita in NJ
Tissue issues
THE TISSUE ISSUE – ADVICE FROM OUR MEMBERS
Puffs are available plain or with aloe cream in them and they seem to shed less than others. Some of the harder finish store brands also shed less. Try several brands and see what works best for you. An environmentally friendly solution to our need to catch a cough or to clean our stomas is to purchase a quantity of low lint cloth handkerchiefs or soft, thin, washcloths. Wash several times to get rid of the lint or dye odors before using.
See below for suggestions from our list:
(1) The only time I use Kleenex is when I am not glued up, and my stoma area is fairly clean (no glue residue); normally, I use a cotton handkerchief, with NO starch. I have used paper towels, toilet paper, catalog pages, old newspapers, and leaves, when in need. None of these do I recommend other than in an emergency. I think paper towels are too rough and like something that is soft, but that will not fall apart. That’s why God invented cotton handkerchiefs.
Philip Clemmons
(2) After one of our returns from our friendly ENT, we had an abundance of NUGauze General-Use Sponges. They are made by Johnson & Johnson and are 4″X4″ and 4 ply. They are available at any medical supply store and come in Qty. of 200. We use these exclusively for stoma care, wash them out with any anti bacterial soap and are reusable for sometimes up to a week. It’s great because they are soft on my Hubby’s skin and everyone knows how tender the area can get. They also don’t create any residue or dust like tissue does.
Maria–caregiver of William
(3) I started out with one of the well known paper towel brands until they changed their consistency and were much coarser and not soft at all. Then, I then switched to Bounty Select-a-Size and have been using them for many years now with no problems.
Jean & Donald Blaisdell
(4) By now you should have figured out that the biggest part of getting on top of this laryngectomy thing is simply mucus management. That stuff just shouldn’t be running down your neck/splattering your mirror or keeping you from enjoying a good breath of fresh air. The former is unsightly and the latter is downright uncomfortable. Most likely, the first thing your friendly ENT or nurse gave you to remedy this situation was a facial tissue and there is very good chance that your are still using them for that purpose. Wrong! Those things are designed for some lady to remove her facepaint or for you to blow your tender, sensitive, formally useful nose. Actually, you may encounter a couple of very real problems using facial tissues for stoma cleaning. First, they are just too light and flimsy making them a fair candidate for inadvertent aspiration. A damp tissue in the stoma? I doubt anyone would want to go there! If that were not bad enough, there is another, equally undesirable, reason for not using facial tissue. Go to a strongly sunlit window and shake your facial tissue. See that little dust-like stuff being ejected into the air by the tissue? Those things are tiny, irritating wood fibers. Every time you place a tissue near your stoma, you give your windpipe a good dose of that. Care to guess what they produce on the vulnerable mucous membranes of your respiratory system? You got it. More protective mucus! You may wish to consider using something a little more substantial like paper napkins or paper towels. I take my wife’s select-a size paper towels, cut them in half and keep about 50-75 in a square, 5 cup sized, Rubbermaid ® serving-saver container that seems to be designed for that very purpose. It doesn’t matter what you use, but you really do need to put those facial tissues down.
Marvin Whitley
(5) My two cents worth goes as follows. You are all right and all wrong. I have used tissue, paper towels, wash cloths, handkerchiefs, napkins, and the same 4×4 gauze pads from the hospital. They all work just fine, as to how much lint is involved, I don’t know. I have settled on the 4×4’s and napkins, Yes plain ole dinner napkins. I feel very secure and safe using these. This brings me to my point, whatever makes you feel the best about yourself is what you should be using. There will never be a universal cure-all solution for all of us, so never be afraid to try something new, TRY them all and go with your heart.
G.W. Buck–Fuzzy
(6) I’m sure I’m going to get into trouble for this reply, but I think all the discussion about paper towels, gauze pads, wash cloths, handkerchiefs and tissues is a tempest in a teapot. Granted, we are all different – and certainly entitled to our own opinion – but I’ve been using Kleenex for over 15 years and I’m wiping up mucus for heaven’s sake which should trap most, if not all, of the lint they generate. I’ve not had a mucus plug since three days after surgery and not had serious mucus problems since I was at the hospital while my wife was getting a new heart valve and I had a full blown case of bronchitis. I see some lint on my “hands free” filter at the end of the day, but have no idea if its source is Kleenex, cats, or house dust. I suspect that there’s more incidental dust in our lives than from a tissue.
Carl Strand ’93
(7) Never thought we’d be having an ongoing conversation about tissues and gauze pads, but it does help to fill up the time between bowl games. Gauze pads were never suggested, and I didn’t want to start laundering handkerchiefs, so I’ve been using the maligned tissues for 10 years. I don’t inhale because that would defeat the purpose, and when I exhale I do it rather forcefully so any lingering lint should be blasted into outer space. That’s my theory and I’m stuck with it.
Mike Rosenkranz ’99
(8) I’m afraid of tissue also. But one thing I have not seen mentioned is the inexpensive wash cloths. The ones that you can buy a stack of them for 5 dollars. They are great around the house and just throw them in the washer/dryer.
Linda Palucci
(9) Here is another possible alternative to the tissue/paper towel issue. Someone had recommended to me that “Puffs” has much less lint than other tissues and a lot less irritating than paper towels. I have been using Puffs ever since. Puffs come in home/office size boxes as well as pocket size packages.
Don Whipple-2000
(10) On searching for as close to a lint free paper towel as I can find I came across a brand called So Dri made by Georgia-Pacific. These have much less lint than Bounty or any other brand I have tried. They are not as soft as some but I use them for cleaning my Lary tube and am not worried about them being “user friendly” but just want something that soaks up the water and leaves as close to a lint free surface as I can get, so these do the job just fine for me.
Wild Bill from Minnesota
(11) For all those messy mucus, and other messes that need swabbing near the stoma, I have been using cut pieces of Good Paper towel, Bounty mostly in select-a-size, (learned from WebW on one of it’s helpful pages) but it takes time to cut them, and convenience is everything these days. I have found that Charmin makes an Extra Strong variety that is almost as lint free as the bounty, but not quite. But it separates into one two or three sheet amounts without cutting, and fast, and accurately. The size is perfect for me. Dust and lint being slight, I believe they are a good back-up, or primary swab to carry with, or have around the house. I stack them up and put them in plastic bags, or just a pocket, or tray.
Steve Israel
ARTICLES
Mucus – Mucous
While my spelling is fairly decent and I have a pretty good eye for words, I did make the mistake early on of spelling mucus, that stuff we are all familiar with, as mucous, which is an adjective, as in, Mucous Membrane (a mucus-secreting membrane lining body cavities and canals connecting with the external air). Mucus, a noun, is the viscid watery secretion of the mucous membranes, that moistens and protects them.
I stumbled across the difference several years ago when I was looking for an exact meaning of mucus for an article I was writing, and did not change it in my usage because mucous seemed to be the more common spelling in use by everyone and, besides, it ‘looked’ right. Not to everyone, it seems, because I received a teasing note from a doctor friend on the Larynx-C email list. Seems he was a spelling champion in school and it has stuck with him. I answered his email that I love words and I know better than to mistreat them so I would immediately start spelling this correctly.
Thought I’d better explain my loss of the “o”, because the next time I write about mucus, that “o” will be long gone!
PWS
Some good tips from Oncolink
Some good common since tips for controlling mucus can be found at the following site:
https://www.oncolink.org/
Thinning Mucus and Saliva
You are unlikely to be around a laryngectomee for 5 minutes without hearing the word mucus and if you get two or more of us together, we talk more about mucus than we do about our new voices.
Excess or thickened mucus is a problem for most of us. It is secreted by the mucus membranes for protection of the esophagus and the trachea. Too little and we are all dried up; too much and we cough it out from the stoma, cough it up from the throat, have trouble swallowing and have trouble talking through it with TEP or ES speech. The thicker it is, the worse our problems become but we can’t be without it, so what do we do? We THIN it.
Saliva, another problem of – too much, too little, or too thick, is a clear, viscous, alkaline secretion from the salivary glands. It will normally decrease as we age and, as it lessens, the sense of taste is affected, speech can be more difficult, food is not digested as well, and overall dental health deteriorates. Saliva contains an enzyme that helps digest food, keeps the mouth moist, and eases swallowing, and it contains antimicrobial and antifungal agents. It is easy to see why we need saliva to stay healthy. In addition, we all know that having a dry mouth is a miserable feeling.
We who have had either chemotherapy and/or radiation, may precipitate these natural “old age” symptoms and our salivary glands might not work as well as they used to, if at all. The amount of damage depends on the type and quantity of chemotherapy or radiation and the fields included in radiation. Some medications, such as antihistamines, will reduce the flow of saliva so we should be careful how many and how often we take these.
We all know about humidifiers, dampened stoma covers, and irrigation, so, what else can we do to help the situation?
If someone told you about a product that is calorie-free, would keep your skin in a healthy condition, lower your risk of urinary cancers and perhaps colon cancer, hydrate your tissues, prevent kidney stones and, very important to laryngectomees, thin mucus and saliva, you would say, “I want some of that medicine. I don’t care what it costs!” That medicine comes right out of your water tap and the cost, even if you prefer to buy bottled water, is one of the cheapest “medicines” around. Feeling tired? You may be dehydrated. Have a few glasses of water! If you wait for thirst, you may have already started to dehydrate.
The problem here is that hardly any of us drink enough water and the only way we can know for sure is to measure. Take a favorite glass and a measuring cup. Don’t cheat. Fill the glass ‘appropriately’ and, pour it into the measuring cup to note how much it takes to fill it to that level. Then it will be easy to calculate how much you are drinking daily. Juice glasses are usually 4 to 6 oz. Tea and water glasses are probably 10oz or 12oz. How many of these do you need? For years we have heard that we should drink 8 glasses of water a day and they are talking about 8 oz glasses. That’s 64 ounces or 1/2 gallon and doesn’t sound so bad if you get to count coffee, tea, and colas, but you can’t count that way. These other drinks are dehydrating so you have to drink more to come out even. Count these drink as about 2/3’s of actual liquid content. A 6oz cup of tea would count as 4oz. Any noncaffeinated beverage counts as water. Foods have water content, but not enough to add much to your list. To make it even worse, Mayo Health says to divide your body weight by half and that’s how many ounces you really need each day. That means the 1/2 gallon would only be enough if you weighed 128 pounds! So, if you weigh 200 pounds, drink 100oz of water a day. Think how important it is to a laryngectomee that water carries oxygen to your cells and helps to thin mucus.
Keep a jug in the refrigerator, carry a bottle around with you, and keep a glass at the kitchen sink. Drink a glass as soon as you get up in the morning and drink water with your meals. Swig a little extra when you take your medicines, especially vitamins, which need water to dissolve and be accessible to your body. Flavor it with lemon or lime or make a juice spritzer with carbonated water. Substitute some Gatorade but no more than a glass or two a day. It was meant for drinking after heavy exercise.
Any moisture that you can put “in”, “on”, or “around” your body will help to moisturize. Use your humidifier, dampen your stoma bib, hold your hot drink up so you are breathing in some of the rising steam, carry the water glass or bottle around with you and sip often. Water is an excellent expectorant and it may be that water alone is the medicine you need for thinning mucus.
There is a medication, an expectorant called guaifenesin, for thinning mucus. It has been approved by the FDA for almost 50 years and is sold both over the counter and by prescription for stronger dosages. It reduces the thickness and stickiness of mucus but must be taken with a full glass of water for it to be most effective.
You will have to read labels of cough syrups, but the one that has just guaifenesin is called Tussin or Robitussin Plain and is 100 mg per teaspoonful. Your doctor might have prescribed this for you, when you were having respiratory problems, under the name Humibid (600mg sustained release tablets usually prescribed 2 tablets in the morning and two at night) or under the generic name G-Bid. If you have trouble swallowing tablets, you might talk with your doctor about Humibid capsules (300mg) that are often called Sprinkles, because you can open the capsules and sprinkle these on your food or in liquid.
Unless your doctor has you on a water restricted diet, you will need to drink a lot of water with or without the medication. Talk with your pharmacist or physician about these suggestions.
by Pat Wertz Sanders (From HeadLines 2000)
 This site is protected by reCAPTCHA and the
This site is protected by reCAPTCHA and the